
A western diamond-backed rattlesnake, which is venomous, is found more commonly as you travel west of the Dallas-Fort Worth area. Photo by Michael Smith.
June 9, 2023
Any opinions in this article regarding first aid and medical treatment are based on the cited guidelines and interviews with physicians. The author is not a physician.
As the weather warms up and people go outside, some people start worrying about venomous snake bites. Such bites are always medical emergencies, but fatalities are rare. Knowing a little about snake behavior can help you avoid being bitten. However, if a person is bitten, it is crucial to know what to do as well as what not to do.
In North Central Texas, we are blessed (some would say) with about 40 species of snakes, only seven of which have a venomous bite that is medically significant for humans. But those seven — the coral snake, copperhead, cottonmouth and four species of rattlesnakes — command a lot more attention than all those harmless ones.
DO SNAKES WANT TO BITE?
 A broad-banded copperhead, which is venomous, is one of two kinds of copperheads found in North Texas Photo by Michael Smith.
A broad-banded copperhead, which is venomous, is one of two kinds of copperheads found in North Texas Photo by Michael Smith.
To any snake in our area, we look big and dangerous. The snake calculates how to survive an encounter with us. Almost always, the first choice is either to stay still and avoid being seen or to try to get away. If they know a good hiding place that happens to be in your direction, they may move toward you — but they’re trying to get somewhere safe, not attack or chase you.
If being invisible or trying to get away does not work, and the snake thinks it’s going to be attacked, it may try to look or sound dangerous (hissing, flattening itself out to look bigger or rattling) and it may try to bite. Many venomous snake bites are really mistakes when we reach or step beside them and the snake assumes we are attacking it.
Some snake bites happen when we are trying to kill it. A person trying to kill a copperhead with a shovel makes the snake frantic to escape or defend itself, and in the process the human may be bitten.
BE PREPARED FOR A SNAKE ENCOUNTER
Hiking or camping at this time of year might result in you seeing a snake. How can you prepare and stay safe? It’s helpful to know which species are venomous and it’s good to have people and transportation in case of any emergency, not just snakes. But leave that snake bite kit on the shelf, it won’t help.
Learning to identify snakes takes lots of practice. You can carry a field guide and you can hang out in “Snake ID” groups on the internet — those things will help. But remember, if you keep some distance between you and the snake, it won’t matter if it’s venomous or not. As you now know, even the venomous snakes want to avoid you and they won’t chase you.
If you keep some distance between you and the snake, it won’t matter if it’s venomous or not.
DON'T RELY ON 'ID RULES'
 A northern cottonmouth, which is venomous, is sometimes called the "water moccasin.” Photo by Meghan Cassidy.
A northern cottonmouth, which is venomous, is sometimes called the "water moccasin.” Photo by Meghan Cassidy.
Don't rely on the so-called “rules of thumb” for knowing which snake is venomous. It’s my belief that very few amateur or professional herpetologists use those rules when in the field. Not only that, the rules are too narrow, misleading and impractical. For example:
• Head shape. Triangular doesn’t necessarily mean venomous. When threatened, many harmless snakes flatten their bodies and heads so that the head may look triangular. The venomous coral snake has a narrow head.
• Eye shape. Venomous pit-vipers have elliptical (cat-eyed) pupils, but not the coral snake. And if you are close enough to an unidentified snake to see whether the pupil is round or elliptical, you are almost always too close.
• Red and yellow colors. If red touches yellow … oh, never mind. When people see coral snakes or milk snakes, they are usually moving and it’s nearly impossible to see if red bands touch yellow bands. And some coral snakes are born with weird patterns that don’t follow the rules.
The best preparation for a safe hike or camping trip includes knowing where you would go and how you would get there if someone was seriously ill, had a broken bone or was snake-bitten. First aid kits are good to have for most injuries, but there’s no reason to carry a snake bite kit as we’ll see below.
Let someone know where you will be, and have a check-in time so they would look for you if you don’t check in. Have a plan for calling for help and then getting there.
The best preparation for a safe hike or camping trip includes knowing where you would go and how you would get there if someone was seriously ill, had a broken bone or was snake-bitten.
FIRST AID ADVANCES
Snake bite first aid has advanced a lot over the years. It was once thought that making a cut into the fang marks would allow you to suck out some of the venom. Now we know that cutting only adds more injury without really allowing much if any venom to be removed. Even the mechanical extractors (a sort of suction cup you would put over the fang mark) remove almost no venom, according to the Wilderness Medical Society’s practice guidelines for pit-viper bites.
Some of the old first aid practices once used to treat snake bite are considered outdated and possibly harmful.
Those same guidelines recommend against tourniquets or pressure bandages. They can do a lot of damage and studies do not show that they help, according to the practice guidelines.
Other strategies like packing the bitten limb in ice or applying electric shock do not help and can be quite damaging, according to the Wilderness Medical Society.
Various guidelines also warn against drinking alcohol or taking aspirin or NSAID medication. A venomous snake bite is generally very painful, but those substances can worsen the victim’s condition.
I spoke with Erik Ledig, MD, an emergency medicine physician with Texas Health Resources who sees patients in the Fort Worth area. He said that few people come in having tried those disproven strategies like cutting, packing in ice, or shock.
“Over time, it’s gotten out there that this is not something to do,” he said.
However, a problem he sees is that people will come in with the snake itself, in the mistaken belief that hospital personnel need to see it.
“Don’t try to catch the snake – we’ve seen injuries from this and delays in treatment.”
A dead snake retains the ability to bite for a while, Dr. Ledig said
“Some of the worst snake bites I’ve seen have been from a dead snake.”
If you can photograph the snake from a safe distance, that can be helpful but is not required.
Guidelines such as those from the Wilderness Medical Society emphasize the following:
• Move away from the snake
• Remove rings, jewelry or constricting clothing from the bitten area because swelling is very likely
• Keep the person calm and reassured
• Get the person to a hospital
HOW SNAKE VENOM WORKS
Snake venom is, from the snake’s viewpoint, primarily a way to subdue their food, and also a good defense when the snake is attacked. The coral snakes have venom that primarily acts on the victim’s nervous system (described as neurotoxic) and venom from some coral snakes can result in weakness, paralysis and the victim may stop breathing. I spoke with snake bite expert Spencer Greene, MD, who is director of toxicology and an attending emergency physician at HCA Houston Healthcare-Kingwood. Dr. Greene said that, luckily, there has never been a death from the variety of coral snake found in Texas.
“In North and Central Texas, some people do get objective weakness,” he said. “What they don’t get is significant weakness leading to respiratory or skeletal muscle paralysis.”
Our other medically significant venomous snakes are the pit-vipers — the copperhead, cottonmouth and rattlesnakes. Their venom primarily destroys tissue, attacking muscles, connective tissue, blood vessels and blood components (described as hemotoxic). Someone bitten by one of these snakes generally has swelling, bruising, pain, problems with blood coagulation and other symptoms. (It should be noted that some populations of a couple of rattlesnake species have venom that is more neurotoxic.)
WHAT HAPPENS IN THE HOSPITAL
The Clinical Practice Statement from the American Academy of Emergency Medicine, co-authored by Dr. Greene, states that for pit-viper bites the affected limb should be elevated (see photo). This helps limit swelling and pain and keeps venom from accumulating in the bitten limb.
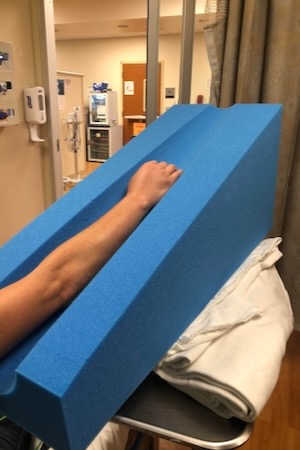 Photo shows the degree of elevation appropriate for a pit-viper bite. Photo by Spencer Greene.
Photo shows the degree of elevation appropriate for a pit-viper bite. Photo by Spencer Greene.
The primary treatment for venomous snake bite is a medication called antivenom (sometimes called “antivenin”) that binds to venom molecules and neutralizes them. It is given intravenously in the hospital under close medical supervision.
When a person bitten by a venomous snake comes into the hospital, a physician evaluates the kinds of symptoms the patient is showing. Treatment depends on those symptoms. For example, someone who was bitten by a rattlesnake might exhibit no significant swelling, pain, bruising and laboratory findings might be normal. After observing the patient for at least eight hours, the physician might conclude that the snake did not inject venom (a so-called “dry bite,” which according to Dr. Greene is very unusual, less than 10 percent of pit-viper bites).
Or, that patient might have swelling that has progressed from the foot where the bite occurred to above the knee. Lab findings might be abnormal and there could be bruising (indicating venom effects on blood and blood vessels) and considerable pain. Such symptoms would call for antivenom to be given, according to the Unified Treatment Algorithm for the Management of Crotaline Snakebite in the United States. That algorithm is an evidence-informed set of medical guidelines that can guide physician decisions about treatment.
Some physicians are conservative about using antivenom, and not every bite will require it. The Unified Treatment Algorithm states that it is not needed if a pit-viper bite produces only localized pain and swelling in a bitten limb, if these symptoms are not progressing (spreading or getting worse). Antivenom is expensive and there are possible adverse reactions, although the risks of allergic or other reactions to antivenom are much lower than they used to be and are not hard to manage.
A helpful way to understand the decisions about giving antivenom is a metaphor used by Dr. Greene. He compares the damage done by venom to the damage done by a house fire. He describes it this way:
“We know that house fires can be extinguished with sufficient water,” said Greene. “We don’t wait for the fire to spread and spread before deciding that now is a good time to use the water, because that way, more damage has occurred and we end up using more water. It’s the same thing with an envenoming. If they have anything more than an insignificant envenomation, we want to treat. We know that even mild bites benefit from treatment with antivenom.”
BE AN INFORMED SELF-ADVOCATE
Because physicians and hospitals vary in how much experience they have treating snake bite, it helps to be well informed and advocate for your own best care. One useful resource for this is the National Snakebite Support Facebook group. Snake bite experts including Dr. Greene volunteer their time to consult with patients and with physician colleagues. If a member posts that they have been bitten, staff can offer information without charge (and other members are not allowed to comment so that it doesn’t become a social media free-for-all). They do not “treat” people via Facebook, of course, but can help make sure you have good information.
Super Safety Saturday
About: For more information, you can come out to the “Super Safety Saturday” hosted by Texas Health Resources at Texas Health Neighborhood Care & Wellness in Willow Park (between Fort Worth and Weatherford). It is a free event covering lots of safety topics. GSDFW reporter, author and herp expert Michael Smith will be there with snake bite information and a harmless, friendly native snake.
When: June 24, 9 a.m. to noon.
Where: Texas Health Neighborhood Care & Wellness, 101 Crown Pointe Blvd. in Willow Park.
Contact: 817-757-1500
RELATED ARTICLES
Snake ID takes practice, cautions North Texas expert
Western rat snakes can spook North Texas homeowners
Cottonmouths have been miscast in tall tales, says Arlington expert
Stay up to date on everything green in North Texas, including the latest news and events! Sign up for the weekly Green Source DFW Newsletter! Follow us on Facebook and Twitter. Also check out our new podcast The Texas Green Report, available on your favorite podcast app.









